
Acne is a common skin concern that affects most of us. However, the underlying causes for acne are different, just like each skin type is unique. Understanding the various conditions that can cause breakouts is crucial for proper care and treatment.
Two common acne types that can often be confused are closed comedones and fungal acne. While they may share some similarities in appearance, they have different underlying causes and require distinct approaches for effective treatment.
In this article, we will delve into closed comedones VS fungal acne, highlighting their causes, symptoms, treatments, and, most importantly, their key differences.
What Is Fungal Acne?
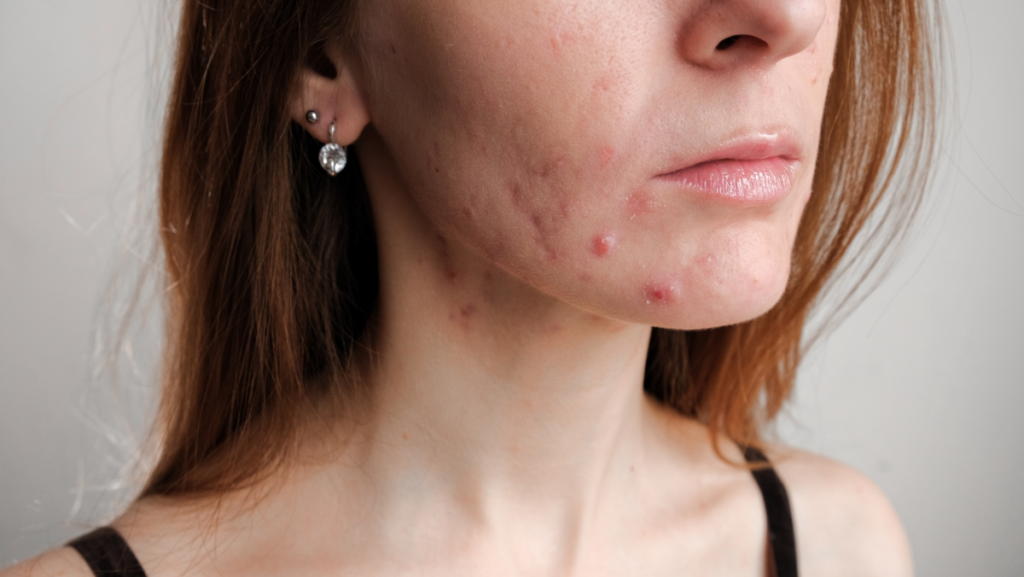
To clear the debate about closed comedones vs. fungal acne, we must understand each one. Since closed comedones are more common and widely recognized, let’s start by unveiling what fungal acne is.
Fungal acne, also known as Malassezia folliculitis or pityrosporum folliculitis, is a fungal infection of the hair follicles that results in the formation of small bumps on the skin.
Normally, our skin harbors a variety of microorganisms, including a yeast called Malassezia. However, when there is an overgrowth of Malassezia that infiltrates the hair follicles, it can lead to the development of pityrosporum folliculitis, a.k.a. fungal acne.
Why Does Fungal Acne Occur?
The primary cause of fungal acne is an overgrowth of Malassezia yeast within the hair follicles. Several factors contribute to this condition, including hot and humid environments, excessive sweating, and skin occlusions.
Furthermore, the disturbance of the natural skin flora caused by antibiotics and steroids can also play a role in developing fungal acne.
It is important to note that specific triggers, such as intense exercise, outdoor work, and occlusive clothing or topical products, can exacerbate flare-ups of fungal acne.
What Are The Symptoms Of Fungal Acne?
The symptoms of fungal acne typically manifest as itchy bumps, which appear uniform in shape and may look like your common whitehead. They may even cause a burning sensation.
These bumps may persist for years if misdiagnosed as acne vulgaris, a common form of acne. Therefore, it is essential to consider the possibility of Malassezia if you go years untreated with the common acne treatments.
Where Does Fungal Acne Most Commonly Appear?
Fungal acne most typically appears in more than one area. It affects the following body parts in order of frequency:
- Face (forehead and chin)
- Upper back
- Shoulders
- Back surfaces of the arms
- Chest
- Neck
Who Is Most Likely To Get Fungal Acne?
Fungal acne can affect individuals of any age and gender. However, it is more commonly observed in adolescents and males.
People who experience excessive sweating or have skin occlusions are also at higher risk. Additionally, living in hot and humid environments increases the likelihood of developing fungal acne.
How Is Fungal Acne Treated?
One of the most crucial differences between closed comedones and fungal acne is their treatment. Not only is the typical treatment for closed comedones ineffective for fungal acne, but it can also exacerbate it!
Therefore, antibiotics and steroids should be avoided because they disturb the skin’s natural flora. This can lead to a flare-up of yeast overgrowth.
Pro tip: Remember that antibiotics can kill bacteria, not yeast. That is why they are effective against common acne vulgaris that has bacterial.
So, how can you treat fungal acne? First, you need to get a diagnosis. Your dermatologist will then prescribe topical and oral antifungal treatments.
Additionally, managing triggers such as hot and humid weather, increased sweating, and occlusive clothing is essential in preventing flare-ups and promoting healing.
What Are Closed Comedones?
To continue on our subject of closed comedones vs. fungal acne, we will now focus on the first.
“Closed comedones” is a more scientific way to refer to the familiar whiteheads. They are a type of acne lesion that develops when a hair follicle or oil gland becomes clogged with excess oil, dead skin cells, and bacteria.
The accumulation of these substances leads to the formation of a closed pore or follicle, resulting in a raised bump with a white or skin-colored appearance.
Closed comedones are distinct from blackheads (open comedones) because they are not exposed to the air. As a result, closed comedones do not undergo oxidation, which is why they do not acquire the dark color commonly seen in blackheads.
Why Do Closed Comedones Occur?
Sebum is an oily substance naturally produced by the sebaceous glands. Also, the hair follicles normally discharge dead cells carried on the skin surface by sebum. So far, so good… Then, why do closed comedones occur?
Closed comedones, a.k.a. whiteheads, occur due to the overproduction of sebum and dead skin cells. Factors such as hormonal changes, genetics, and certain skincare products can contribute to this, leading to the development of closed comedones.
What Are The Symptoms Of Closed Comedones?
The main symptom of closed comedones is the appearance of small, flesh-colored or white bumps on the skin. These bumps are typically not inflamed or painful.
Where Do Closed Comedones Most Commonly Appear?
Closed comedones are typically found in areas with high concentrations of sebaceous glands, such as:
- Forehead
- Nose
- Chin
- Upper back
- Chest
How Are Closed Comedones Treated
Treating closed comedones involves a multi-faceted approach to address the underlying causes and unclog the pores.
Topical treatments containing ingredients like salicylic acid, benzoyl peroxide, or retinoids are commonly used to exfoliate the skin, reduce oil production, and promote the shedding of dead skin cells.
Regular cleansing, gentle exfoliation, and avoiding pore-clogging products can also help prevent the formation of closed comedones.
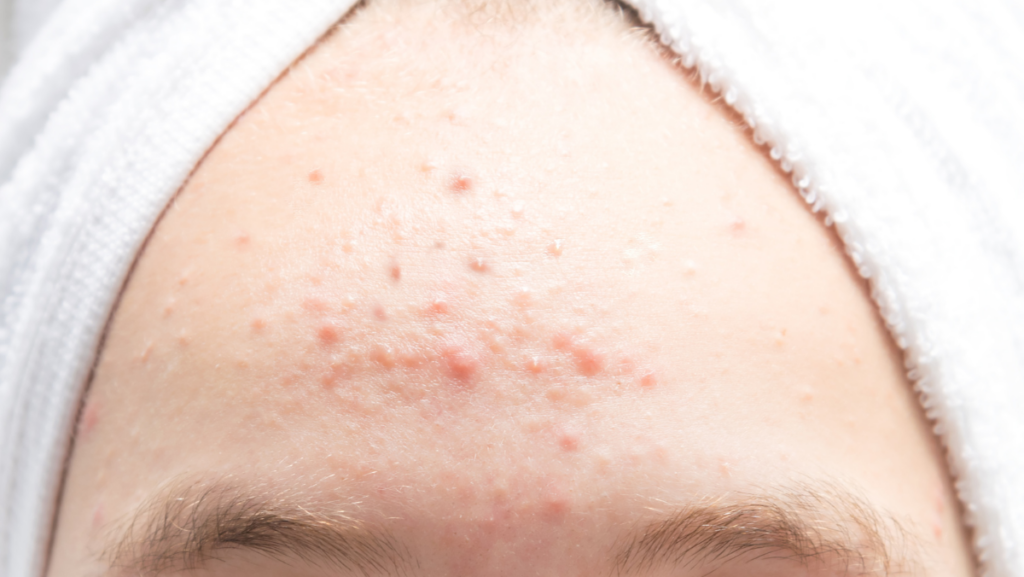
Closed Comedones VS Fungal Acne: What Are The Differences?
So, now that you have become an expert in recognizing closed comedones and fungal acne, we can make a side-by-side comparison to help you tell them apart.
Let’s sum up the differences between closed comedones and fungal acne:
| Closed Comedones | Fungal Acne | |
| Cause | Overproduction of sebum and dead skin cells | Overgrowth of Malassezia yeast within hair follicles |
| Appearance | Small, flesh-colored, or white bumps | Small bumps that resemble whiteheads |
| Symptoms | Non-inflamed, painless bumps | Itchy bumps that may cause a burning sensation |
| Who Is Most Likely to Get it | Common among individuals of all ages and genders. Most commonly during adolescence. | More commonly observed in adolescents and males, people experiencing excessive sweating or occlusions of the skin. |
| Treatment | Topical treatments (e.g., salicylic acid, benzoyl peroxide, retinoids); regular cleansing and avoiding pore-clogging products | Topical and oral antifungal treatments; |
Conclusion On Closed Comedones VS Fungal Acne
Differentiating between closed comedones and fungal acne is essential for effective skincare and treatment.
Closed comedones, also known as whiteheads, occur due to the overproduction of sebum and dead skin cells, leading to clogged pores. They can be treated with topical treatments containing ingredients like salicylic acid or retinoids, along with regular cleansing and avoiding pore-clogging products.
On the other hand, fungal acne, or pityrosporum folliculitis, is a fungal infection caused by an overgrowth of Malassezia yeast within hair follicles. It appears as small bumps that resemble whiteheads and can be accompanied by itching and a burning sensation.
Treating fungal acne requires a different approach, including topical and oral antifungal treatments and managing triggers such as hot and humid weather and occlusive clothing.
Understanding the key differences between closed comedones and fungal acne is crucial to avoid misdiagnosis and ensure appropriate treatment.
Consulting a dermatologist or healthcare professional for an accurate diagnosis is recommended. By implementing targeted skincare routines and using the right treatments, individuals can effectively address these acne conditions and achieve clearer, healthier skin.
Frequently Asked Questions
How we reviewed this article
- Process
😀